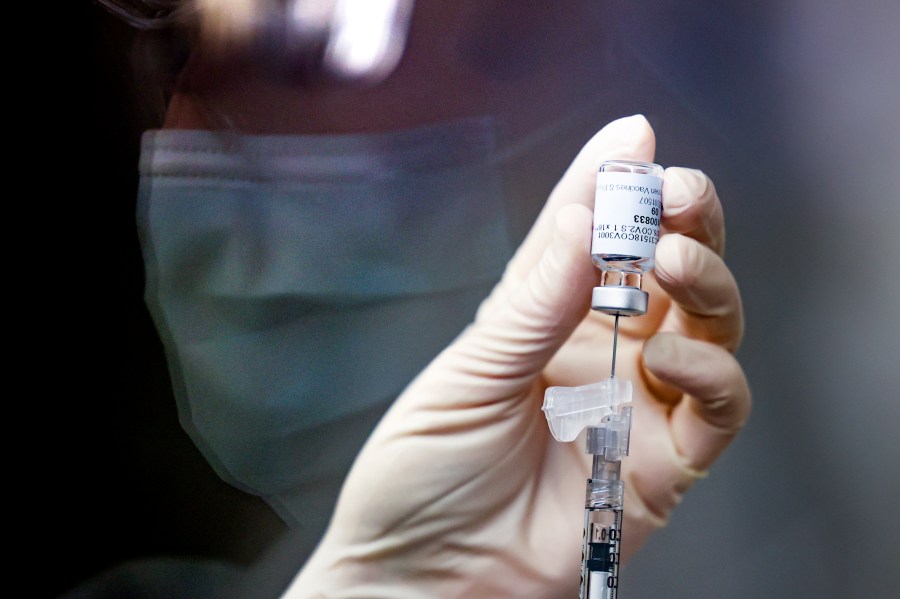
It was just about a year ago that many Americans were breathing a sigh of relief with their gazes solidly fixed on that thing we call “normal.” Many Americans had received their second dose of a COVID-19 vaccine (or their single dose for those who opted for a J&J shot), and it seemed like vaccination was the key to throwing your masks and your worries away.
Of course, in late 2021 the Omicron surge came to the US, and with it the concept of “breakthrough cases.” Health experts struggled to correct expectations that the vaccines should protect against all symptoms, not just severe illness, hospitalization, and death, as the Omicron variants managed to evade vaccine-induced immunity. Now a new booster shot, one specifically designed to target Omicron strains, is here and scientists are hopeful that this will better protect recipients from the current dominant variants and future variants.
Keeping track of what is available and when you should sign up for your next appointment can be overwhelming, but we’ve got you covered. Read on to learn about what boosters are available, how the vaccine distribution effort is changing, and get answers to your questions about the safety of these immunizations.
Editor’s Note: As we’ve witnessed since March 2020, information regarding the COVID-19 pandemic is constantly changing — and the latest on the vaccines is no exception. While we aim to keep our articles as up-to-date as possible, please be sure to check the Centers for Disease Control and Prevention (CDC) website as well for the latest news. Curious about how the COVID-19 vaccines were created? We’ve covered that in How Was the COVID-19 Vaccine Developed?
How Are Experts Accounting for COVID-19 Variants?
The emergence of variants isn’t surprising: it’s well-established that RNA viruses like SARS-CoV-2 mutate frequently. Many mutations don’t have major impacts on how transmissible the virus is or how severe of illness it causes. When mutations cause significant changes in how the virus acts, the World Health Organization lists that variant as a “variant of interest”. When variants of interest begin to spread widely, and cause more breakthrough cases or reduce the effectiveness of public health measures, these variants are classified as “variants of concern”. Variants that are more transmissible will undoubtedly lead to more hospitalizations and strain on the healthcare system.
At the time of this writing, the Omicron variant (including its many sub-variants) is the only variant of concern according to the WHO. There are no variants of interest at present. Of course, you can easily check for yourself whether or not the situation has changed by checking the WHO’s COVID-19 tracker.
The rise of the Omicron variant also signaled a shift in how we understood vaccine efficacy, as the variant managed to evade vaccine-induced community and cause illness even in vaccinated individuals. Now, booster shots are being produced to target new variants of concern.
Variant-Specific “Bivalent” Booster Shots
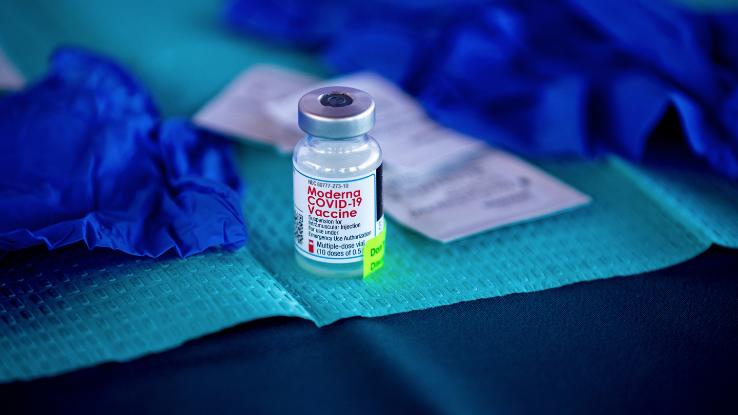
In August of 2022 the U.K. became the first country to approve an Omicron-targeted booster shot. Known as “bivalent” vaccines, these shots blend vaccine formulas designed to target the original COVID-19 virus with a new formula specifically designed to fight off infections caused by the Omicron variant. As the virus continues to evolve, it looks less and less like the original. By creating vaccinations that target a more evolved variant, the hope is that these vaccines will also protect against future variants, that are likely to more closely resemble newer variants than the original virus.
In the United Sates, the FDA also just approved a bivalent booster, specifically formulated to target the BA.5 strain (a more recent Omicron strain) which is currently dominant in the States. The hope is that this new formula will be even more effective than the one just approved by the U.K. at protecting Americans from both the BA.5 variant and whatever variants are likely to evolve after it.
When Should You Get Your Next Booster Shot?
While it might seem like the sooner you can get your booster the better, the CDC has specific guidance for you to follow in order to assure optimal protection. In fact, studies suggest that getting booster shots too close together or too soon after you’ve been infected could reduce the efficacy of your booster. General guidelines suggest that adults aged 18 years and older may want to delay their booster shot for 3 months after being infected with COVID and should wait at least 2 months after their last booster before getting another. Of course, you should always consult with your doctor about the best time for you to get your vaccinations, especially if you are older, at higher risk of severe infection, or are figuring out the right timeline for your child’s vaccinations.
Not All Boosters Will Continue To Be Free
The Biden administration is planning to buy the aforementioned bivalent boosters. You can expect to see access to those rolling out in early-mid September, according to White House Covid-19 Response Coordinator, Dr. Ashish Jha. However, funding for the purchase of this new batch of vaccines is being cobbled together from a few places, as additional federal funding didn’t pass in Congress. This means that soon Americans will see the commercialization of vaccines, tests, and treatments. You shouldn’t expect to pay much for your COVID-19 care through this fall, but come early 2023, that is likely to change.
How Is the COVID-19 Vaccine Rollout Going Overall?
The vaccine rollout started in the U.S. on December 14, 2020. As of August 22nd, 2022, the CDC reported that approximately 224 million people — including both adults and children over age 5 — were fully vaccinated and with over 100 million people having received at least one additional booster dose. In total, around 608 million doses were administered. In October of 2021, the FDA authorized emergency use of the Pfizer-BioNTech vaccine in adolescents ages 5-11 — an expansion that FDA Commissioner Dr. Janet Woodcock said will “bring us closer to returning to a sense of normalcy.”

As of August 2022, about 80% of the total population has received at least one dose of vaccine. Ninety-two percent of individuals aged 65 and up are fully vaccinated, and 30% of children ages 5-11 are fully vaccinated. But vaccination rates have experienced very slow growth since July of 2021, and vaccine hesitancy is impacting adults’ decisions to vaccinate themselves and their decisions about whether or not to vaccinate their children. A recent Gallup poll found that 57% of parents with children under the age of 5 do not plan to vaccinate their child. Still, vaccination rates globally continue to climb, which is critical to slowing the emergence of new variants.
Is the COVID-19 Vaccine Safe?
As Symptomfind notes, the vaccine has been deemed both safe and effective. Before a vaccine is deemed safe, it goes through what the CDC calls “rigorous” testing from both developers and the FDA.
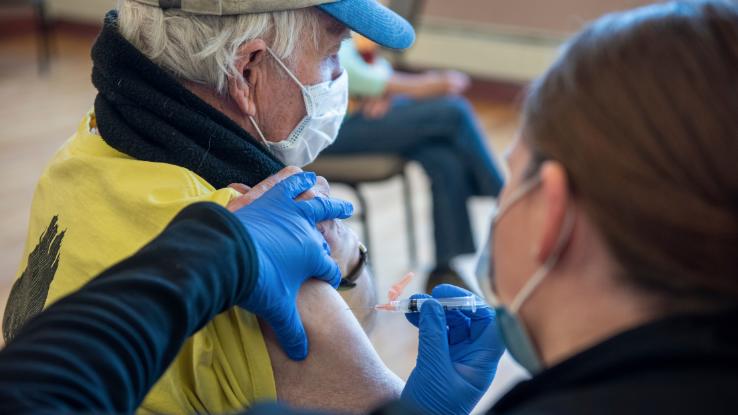
A variety of myths about vaccine safety still persist, more than a year after the initial vaccine rollout. Some of these myths include that the vaccine will negatively affect fertility in people with uteruses, and that the vaccine was rushed through the development process and therefore not adequately tested for safety. The popular Gimlet Media podcast Science VS dedicated an entire episode to fact checking a controversial Joe Rogan broadcast on Spotify that spread a considerable amount of disinformation.
Some of the myths that permeate the discourse are more easily spotted than others. We’re written up a handy guide to help you spot misinformation and disinformation. One common and understandable fear shared by some Americans is that the vaccine will actually make them sick — so what’s the deal there? “No matter the vaccine — and no matter what a vaccine is fighting against — injection is often accompanied by mild side effects, including fatigue, swelling, pain, and redness at the injection site, all of which usually clear up within 24 hours,” our colleagues at Reference found. “In fact, these types of side effects ‘show that the vaccine is working, because it stimulates the immune system and the body forms antibodies against the infection that is only ‘feigned’ by the vaccination.'”
The bottom line? Getting vaccinated doesn’t mean you’re completely immune to contracting COVID-19, but it will help protect you against contracting a serious illness or ending up in the hospital. The efficacy rates of the vaccines are impressively high, and the CDC continues to update its guidelines for fully vaccinated and unvaccinated individuals, as well as updating recommendations for booster shots.
Does Getting Vaccinated Mean Life Can Return to “Normal”?
In short, no. In the early days of the pandemic, a “return to normal” was the carrot that public health officials dangled to convince the public to mask up and lock down (remember when we were told that we just needed to “flatten the curve”?). As with “flattening the curve” the messaging has changed, and “normal” needs to be replaced with “new normal.”

The prospect of herd-immunity, once held up as a possible path to ending the pandemic, has largely been rejected as a possibility at this point by leading scientists.The coronavirus is here to stay, and now our focus needs to be on what an endemic coronavirus will look like. In other words, we will always be living with the virus, but the public health measures we collectively take now can still have a big impact on how dangerous and deadly the virus continues to be. And a robust and ongoing vaccine effort is one of the most impactful measures on that list.
Additionally, The CDC regularly releases updated guidelines for people who are fully vaccinated, partially vaccinated, and completely unvaccinated. One sentiment remains constant – people must continue to take the recommended protective precautions to reduce the spread of COVID-19.
Learn More About the COVID-19 Vaccines
These articles and resources can help you learn more about a variety of topics related to the COVID-19 vaccines.







