In the wake of immense public pressure, the Food & Drug Administration’s (FDA) ban on blood donations from gay, bisexual and queer men took effect in the 1980s amid the AIDS epidemic in the United States. Almost four decades later, the ban still holds, even with the U.S. facing its first-ever blood shortage crisis. While there have been notable changes to the policy — including a modification of the restrictions in 2015 to allow queer men to donate blood if they stayed abstinent for at least a year (later, in 2020, revised to three months) — it’s still not enough.
Following the influx of hospital patients in dire need of blood during the COVID-19 pandemic, pressure has been mounting on the FDA yet again. In January 2022, 22 U.S. Senators joined activists and organizations that advocate for the LGBTQ+ community, in speaking out. These critics called for the end of the three-month celibacy requirement for gay, bisexual and queer men and further encouraged the FDA to lift what now seems like an unfair and unreasonable lifetime ban on otherwise eligible and willing blood donors.
Organizations like GLAAD, a self-described “media monitoring organization, founded as a protest against defamatory coverage of [queer and trans people]”, have called the FDA’s policy outright discriminatory. In 2020, GLAAD even put forth a petition, asking the FDA to repeal the ban.
This isn’t the ‘80s. We know so much more now. And it’s been 40 years since the first five cases of what would be called AIDS were reported. Yet, the long-standing restrictions remain in effect. With the blood shortage crisis impacting the U.S., why can’t we find a compromise that allows men to donate blood, no matter their sexual orientation or sex life?
Here, we’re taking a look at why the lifetime ban is so harmful, and what can be done to encourage the FDA to repeal this discriminatory policy.
Why Can’t Gay, Bi and Queer Men Donate Blood?
In light of the HIV and hepatitis B epidemic in the 1970s and ‘80s, health experts realized these conditions could be transmitted through blood. That said, it was crucial that people at an increased risk of the virus — in this case, men who have sex with other men (MSM) — decreased their chances of passing it to others.
Since effective screening wasn’t reliable at the time, the FDA decided to restrict blood donations from gay and queer men. But, four decades later, our understanding of HIV/AIDS has expanded, and our medical technology has become more reliable. So, why hasn’t the ban changed with the times, too?
As of 2022, the FDA guidance entitled “Revised Recommendations for Reducing the Risk of Human Immunodeficiency Virus Transmission by Blood and Blood Products” states that all U.S. blood-collection organzations must: “Defer for three months from the most recent sexual contact, a man who has had sex with another man during the past three months.”

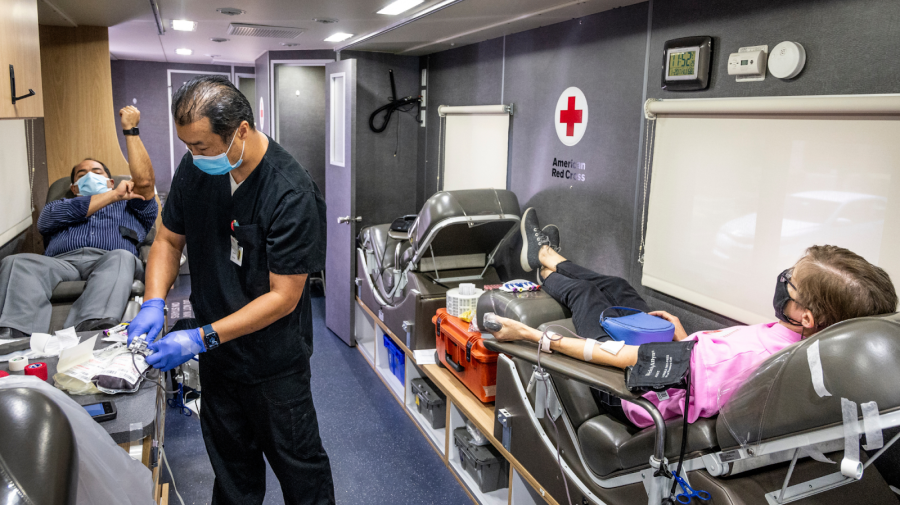
Many of the organizations that run blood drives hold beliefs that are in conflict with the FDA’s rule. “[We] believe blood donation eligibility should not be determined by methods that are based upon sexual orientation,” the American Red Cross states. The blood-collecting organization also notes that putting energy toward research and data can help convince the FDA to change its harmful policy.
Reasons to Allow MSM to Donate Blood
An Outdated and Harmful Policy
From a medical point of view, restricting gay and bisexual men from exercising the right to donate blood seems strange, especially given the severe blood shortage. Adhering to restrictions developed in the 1980s — restrictions developed with limited scientific evidence — isn’t standard practice in the medical field.
After all, we’ve come a long way in the areas of science and technology since the 1980s, and we’ve reached tremendous milestones when it comes to understanding the epidemiology of HIV. Now, the advanced tools at our disposal can safely and effectively screen blood products, for example.
This combination of modern science and innovative tools allows us to diagnose people with HIV and get real-time results. Practitioners can now perform blood tests and ascertain whether a potential donor is infected with the utmost sensitivity. In fact, these diagnoses can be performed by an expert, but people can now perform these tests, in the comfort of their homes, too. So, with such processes in place and accessible now, the ban seems outdated. If our technology has improved and our knowledge has grown, why hasn’t the FDA’s policy shifted alongside these changes?
Other Countries Are Increasingly Allowing Gay, Bi and Queer Men to Donate Blood
As the United States sticks to outdated precedent set by the FDA, many other countries are moving toward — or considering — getting rid of restrictions that prevent MSM from donating blood. Several other nations are, like the U.S., lessening the strictness of their long-standing policies. In short, governments and organizations around the world are realizing that preventing MSM from donating blood is unethical.
So, what are these countries doing to ensure safety and health standards are met when it comes to blood collection and donation? Well, many are changing their screenings and adopting smart risk behavior-based approaches. For instance, individuals recently involved in activities that increase the risk of contracting HIV and other blood-borne pathogens — such as getting a tattoo — are restricted. In other words, it’s your self-reported behavior that restricts you from donating blood — not your identity.
All People Are at Risk of Contracting HIV
Since HIV is a sexually transmitted virus, any sexually active person is at risk, no matter their gender or the gender(s) of their partner(s). Today, more than 38 million people live with HIV worldwide. Even though HIV rates are disproportionately higher in gay and bisexual cis men than in heterosexual people and cis lesbian and bisexual women, restricting MSM from donating blood based on this history comes with a lot of weight.
Not only does the restriction feel like a gender-specific issue, but it’s also deeply rooted in homophobia. During the 1980s and through the early ‘90s, the HIV/AIDS Epidemic in the U.S. wasn’t given much media coverage. When it was covered, the media spread misinformation or cast additional stigma on gay men, trans people, Black people and people of color, and sex workers.
In fact, the lack of coverage, paired with a lack of federal support or consideration, led to it becoming an epidemic of such scale and tragedy. Larry Speakes, then-President Ronald Reagan’s press secretary, laughed about the HIV/AIDS epidemic with the media, dubbing it the “gay plague” and cracking other homophobic jokes. Much of this stigma persists today.
Additionally, while MSM have been more predisposed to the risk of HIV, epidemiologically speaking, there were (and are) many factors at play. For example, the types of sexual relationships a person has — be they monogamous, polyamorous, ethically non-monogamous or otherwise — as well as their safe-sex practices (or lack thereof) all factor into their risk of HIV infection.
The Restriction Reinforces Stigma, Forces People to Lie
Having measures that define who can and who cannot donate blood based on their identity is disincentivizing, to say the very least. Many people who participate in blood drives are involved in high-risk behavior, from intravenous drug use to getting tattoos and piercings to being a sex worker. Still, these donors can still support blood-collecting organizations thanks to the blood screening processes.

Even if a gay man doesn’t engage in so-called high-risk behaviors — he doesn’t use drugs, visit the tattoo or piercing parlor, engage in unsafe sex or sex work — he’s still disqualified based on his sexual orientation. In some ways, then, the restrictions worsen the stigma many in the U.S. still hold toward gay and bisexual men.
Blood donation is essential. Saving someone’s life often boils down to an individual’s willingness to donate blood in the first place. Since you’re required to self-report if you’ve recently engaged in the above “high-risk behaviors” or if you’re a MSM before donating blood, there’s a possibility that some would-be donors may feel compelled to lie. After all, no one should have to disclose personal information, including their sexuality, just to donate blood or receive healthcare services.
The Bottom Line? Make Blood Donations More Accessible and Inclusive
Blood donation is a crucial part of healthcare. For this reason, maintaining a steady supply of blood by encouraging as many people as possible to participate in blood donation is vital; a blood shortage crisis, like the one we’re experiencing now in the U.S., is highly preventable.
The FDA’s restrictions on MSMs are clearly discriminatory in that they bar a particular group from exercising their choice to donate blood. Not to mention, the justifications for the restrictions are outdated and unreasonable. If allowed to donate blood without sexuality-based restrictions, gay, bisexual and queer men could play a substantial role aiding our healthcare industry and helping us navigate the public health crisis that is the blood shortage.
Improved diagnostic and blood screening procedures already make it possible for millions of people who were once banned to donate blood safely. Banning a particular group from donating blood, especially when a simple screening could determine the safety of their donation, is unethical — and only creates further barriers to safe, accessible, equitable and inclusive healthcare.






